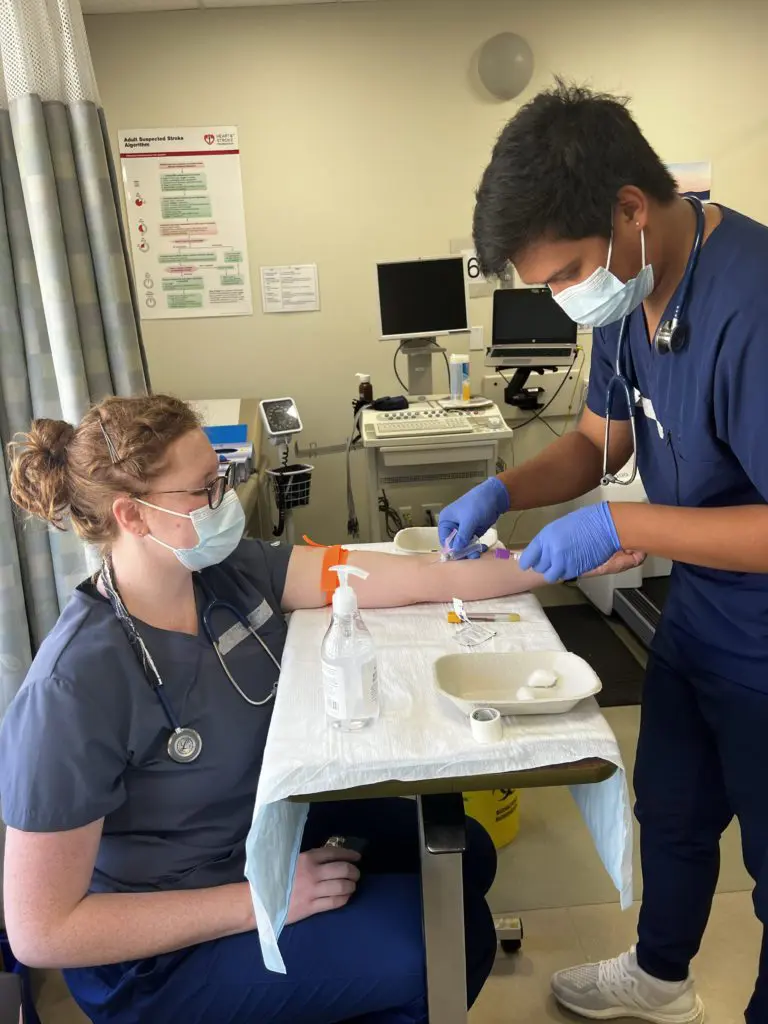
Hi everyone! I hope you are well. Time is flying by as usual, and there have been lots of studying and changes to prepare for my upcoming clinical preceptorship. But I’m already getting ahead of myself – first, let me catch you up to speed with what I’ve been up to for the past two months!
I last left off when I returned from my second lab block in Calgary, where we learned about treadmill stress tests and Holter monitor scanning. Just like our first lab block experience, the purpose of the lab was to integrate our theoretical knowledge into practical applications in preparation for our Integrated Practical Experience (IPE) days in the hospitals or clinics in our hometown. The second lab block was all about exercise treadmill stress tests and Holter scanning, so naturally, our last three IPE days focused on those skills.
Administering the treadmill stress test
For two days, I shadowed the Royal University Hospital Cardiology Technologists administering the treadmill stress tests. I observed how they greeted, prepped, and brought patients to the testing area. A Cardiologist is always present to supervise the testing, with two Cardiology Technologists running two tests simultaneously. Once the doctor has chatted with the patient to collect their health history, the Technologist connects the ECG leads to the patient’s electrodes, which are extra sticky to stay affixed despite movement and sweat. The procedure is re-explained to the patient, allowing them to ask any last-minute questions before the test begins.
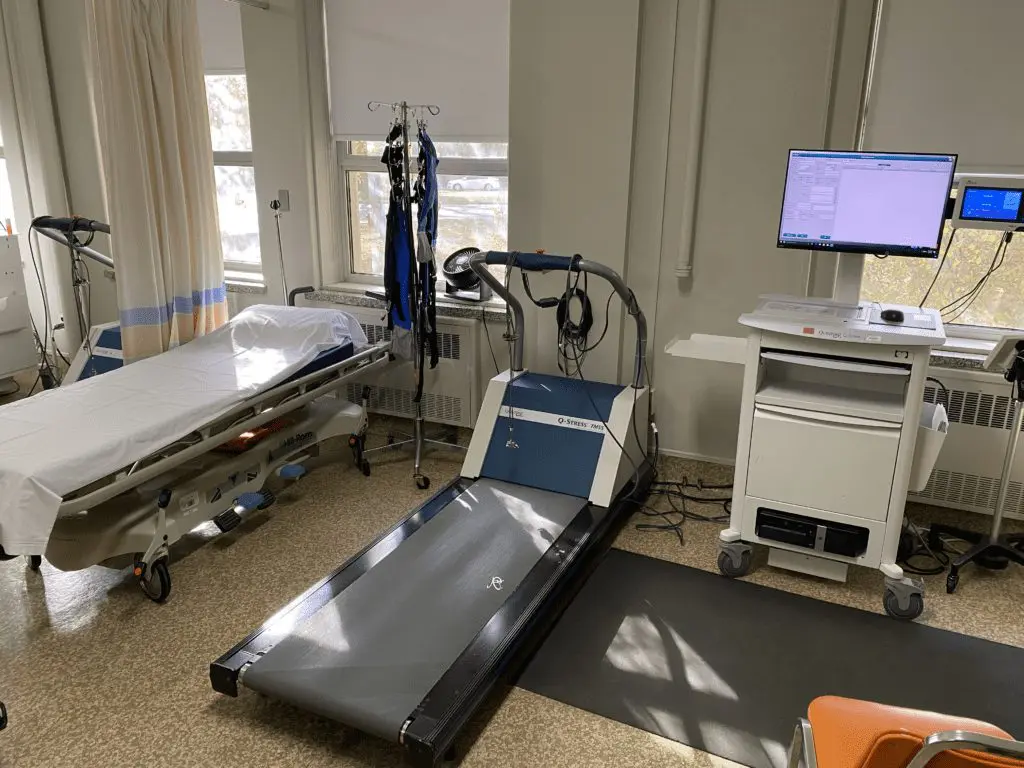
The specialized ECG program monitors the patient throughout the test, and an automated blood pressure cuff takes readings at each stage. The first stage starts with a walk, and as the test progresses, the treadmill increases in speed and incline. The Cardiology Technologist continually checks in with the patient to see if they are starting to experience any chest pain with the exercise and watches the monitor for any changes or abnormalities on the continuous ECG. The blood pressure readings provide information on any abnormal blood pressure spikes or drops with exercise. The test aims to determine if there are any arrhythmias or ST-segment changes that may correlate to the patient’s symptoms. If the test shows no significant changes, it will be terminated because either the patient cannot continue or the doctor discontinues the test. The patient is immediately put into recovery and rests as the ECG and blood pressure readings continue their monitoring. As the patient recovers, the doctor analyzes the data, charts the information, and discusses the results with the patient. Once fully recovered without showing any symptoms (if expressed during the test), the Cardiology Technologist disconnects the patient from the leads and sends them on their way.
During the two days of treadmill testing, there was quite a variety in age and health histories of the patients, ranging from 18 years to the mid-80s. While it is common for older patients to have treadmill exercise tests to investigate symptoms such as chest pain, tests for younger patients may be to try and determine the cause of fainting or shortness of breath. A doctor will administer a treadmill test on younger individuals if there is a familial history of sudden cardiac death. An exercise test ensures the heart is not at risk of starting a rate-related fatal arrhythmia.
An adrenaline-pumping day in the ER
![An ECG demonstrates the extensive antero-septal-lateral myocardial infarction [heart attack] that Taryn witnessed.](https://stenbergcollege.com/wp-content/smush-webp/2022/12/ecg-1024x530.jpg.webp)
One day, during a lull between treadmill tests, one of the Technologists took me to respond to an incoming patient reportedly having a heart attack. We hustled down to the ER, put on our PPE in preparation, and joined a team of nurses and doctors awaiting the patient’s arrival. We didn’t have to wait long before the paramedics rolled in the patient. While the lead paramedic was summarizing the patient’s symptoms and treatment, the team, which included Cardiology Technologists, began the initial assessment. Since the room was bustling with people, I stood by the ECG machine, observing how the Cardiology Technologist deftly stickered and hooked up the patient to the ECG leads, working around everyone else tending to the patient. Once the reading was clear, I hit the record button to capture the ECG tracing. Because the patient had been displaying signs of cardiac distress, it was imperative to complete a clean ECG tracing quickly so that the attending doctor could better assess the patient’s condition. As soon as it printed, we disconnected from the patient, passed the tracing to the doctor, and left the treatment room to make way for more nurses.
Although intense, this experience was a great snapshot of how critical it is to obtain a clear ECG tracing quickly in emergency cases. As suspected, the patient was having an extensive heart attack, indicated on the ECG by ST-elevation in multiple leads. I was grateful that I saw how a Cardiology Technologist worked as part of a trauma team. The Technologist I was shadowing shared advice on how we can’t be shy when entering a crowded treatment room. She joked that sometimes we can’t be afraid to “throw elbows” to get in there for an ECG tracing ASAP, as a few minutes can make all the difference in patient treatment and clinical outcomes. This event definitely added some excitement and adrenaline to my day!
The importance of Holter monitors
While not as an adrenaline-pumping experience as “my first heart attack”, my IPE day focusing on Holter monitors demonstrated the value of this method of cardiac testing. I learned how to prep the patient’s skin to place the extra sticky electrodes and educate them on the proper procedure for wearing their Holter monitor. The purpose of the Holter monitor is to continuously record the patient’s heart rate and rhythm for 24, 48, 72, or 168 hours to ascertain if the heart has any arrhythmias connected to patient symptoms. Once the patient has finished the prescribed time to wear the Holter, they bring the device back to the hospital, where Cardiology Technologists upload and scan the data.
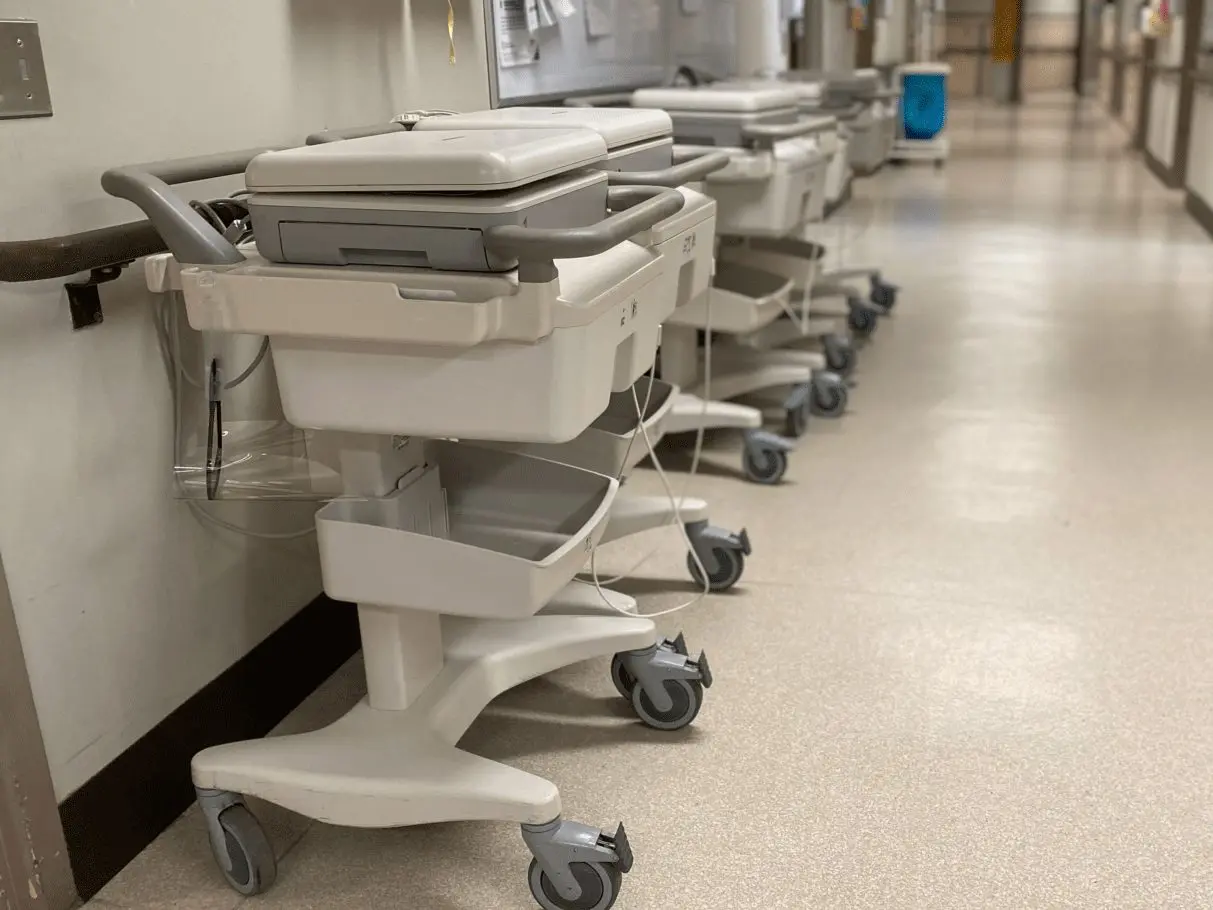
Finishing these IPE days makes me even more excited for what my clinical preceptorship will bring! I can’t wait to be in the hospital daily, honing my skills, and expanding my knowledge in ECG interpretation. As we speak, I’m packing my bags to head off to Regina (another city in my home province), where I’ll complete my clinical between two hospitals over the next three months. It’s hard to believe that it’s been a year since I started schooling. The past year’s hard work, studying, and learning theory have culminated in this moment of embarking on my clinical preceptorship. While I’ll do my best to live in the moment and absorb as much information and knowledge as possible, I know the upcoming months will continue to fly by on my journey to becoming a Cardiology Technologist.

![An ECG demonstrates the extensive antero-septal-lateral myocardial infarction [heart attack] that Taryn witnessed.](https://stenbergcollege.com/wp-content/smush-webp/2022/12/ecg.jpg.webp)